 During the initial consultation, a detailed infertility workup is undertaken and an individualized and patient tailored plan of management is charted out. A comprehensive fertility assessment package is also offered at EFC where besides the fertility consultation, the following investigations are conducted:
During the initial consultation, a detailed infertility workup is undertaken and an individualized and patient tailored plan of management is charted out. A comprehensive fertility assessment package is also offered at EFC where besides the fertility consultation, the following investigations are conducted:
• Hormone assays (D2/3 FSH, LH, TSH, prolactin, AMH*)
• Pelvic ultrasound
• Semen analysis
At our IVF Center We provide a thorough explanation of the diagnosis and the various treatment options to the couple so that they can choose between the best fertility treatment options available to them.
An array of investigations are undertaken to ascertain the cause of infertility before embarking on the journey of fertility treatment (IUI, IVF or ICSI). These include:
• Semen analysis
• Hormone assays (D2/3 FSH, LH, TSH, prolactin, AMH)
• Pelvic ultrasound
• Mid luteal progesterone levels
• Tubal assessment (HSG or SSG)
• Routine investigation e.g. FBC, blood sugar, urine analysis, Paps smear, cervical swabs for culture, semen culture, HBsAg, HIV, VDRL, Blood grouping
• Endometrial biopsy to rule out Tuberculosis
• Hysteroscopy

Most women produce a single egg during a natural menstrual cycle. In order to maximize the chances of success, the goal in an IVF/ICSI cycle is to produce a larger number of eggs by ovarian stimulation using injectable fertility drugs. There are several different types of fertility drugs, which may be administered in different ways and as a part of different drug regimens or protocols.
The protocol best suited for your treatment will be discussed with you in detail by our consultant, and a final treatment plan will be charted out to accommodate any special needs.
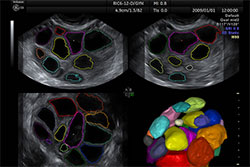
The progress of your cycle will be monitored by a combination of serial ultrasonography and blood tests for hormones in order to:
• Ensure adequate growth of follicles
• Facilitate dosage manipulation of injectable drugs
• Prevent ovarian hyperstimulation (OHSS)
• Time the trigger for final egg maturation in order to optimize egg recovery, and thereby determine the best time for egg collection
This is an injection containing the hormone hCG, which triggers the final maturation of the eggs when they are ready for collection. Egg collection will be performed approximately 36 hours after the hCG injection.
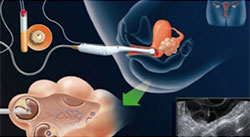
Egg collection is a day care procedure conducted under general anaesthesia, which takes about 20-30 minutes. The eggs are retrieved using a vaginal ultrasound procedure. The patient is admitted in the morning of egg collection, and is discharged on the same evening approximately 4 hours after the procedure.
A semen sample is usually collected on the morning of egg collection, and after sperm preparation and washing, used for inseminating the eggs (IVF) or injecting the eggs (ICSI).
It is essential to remember that the semen sample is of optimum quality after 2-3 days of abstinence. We would therefore advise you to abstain from ejaculation for 2-3 days prior to the day of egg collection.
Surgical sperm retrieval (SSR), when required, is performed by an andrologist under appropriate anaesthesia.
SSR:
• PESA – aspiration through skin
• TESA – aspiration through testicular tissue
• TESE – sperm extraction from testicular biopsy sample
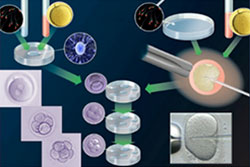
The recovered eggs are put into a special culture medium and kept safely in an incubator to provide the optimum environment. Depending on the sperm count, motility, morphology and few other factors, insemination of eggs may then be performed by either IVF or ICSI.
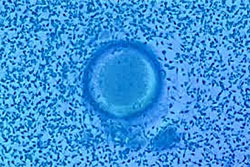
A semen sample suitable for IVF is mixed in appropriate concentration with the eggs and the process of fertilization occurs naturally in culture conditions.
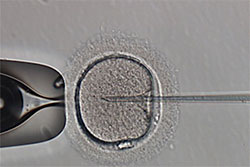
ICSI involves injecting a single sperm directly into an egg, thereby facilitating fertilization. Semen samples with low count, low motility, poor morphology and SSR require ICSI.
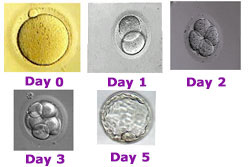
A fertilization check is performed approximately 16-18 hours after insemination. Usually, approximately 80% of the eggs collected are mature, and 60-70% of these mature eggs fertilize. A day 2 check is performed approximately 24 hours after fertilization check. On day 2, embryos should contain 2-4 cells, and by day 3, 6-8 cells.
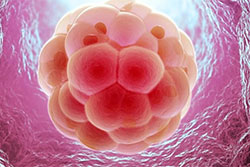
Luteal phase support involves the use of hormone progesterone to prepare the lining of the womb for embryo implantation. Progesterone is started following egg collection in the form of progesterone gel, pessaries, tablets or injection. It is important to continue this till the pregnancy test.
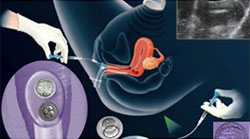
Embryo transfer is a short and simple procedure, taking approximately 15 minutes, after which the patient is free to go home after a short waiting period. The cervix is exposed using a vaginal speculum and a very fine catheter is passed through the cervix into the womb to place the embryos. Optimal placement of embryos is confirmed by an ultrasound scan.
A blood and urine test to check for pregnancy will be performed 16 days after embryo transfer. A repeat test may be required in some cases.
If the pregnancy test is positive, we will give you an appointment for a pregnancy scan (ultrasound scan) to confirm the heartbeat in an ongoing pregnancy.